Understanding the Three Common Anorectal Conditions:
Piles (Hemorrhoids):
- Bright red blood on toilet paper or in the toilet bowl
- Painless bleeding during bowel movements
- Itching or irritation in the anal region
- Pain or discomfort (especially in external piles)
- Swelling or a lump around the anus
- Sensation of incomplete bowel evacuation
Anal Fissure:
- Persistent drainage of pus or blood from the anal opening
- Recurrent anal abscesses
- Skin irritation around the anus
- Pain that worsens with sitting or bowel movements
- Fever and general malaise (if infected)
- Swelling and redness around the anus
Anal Fistula:
- Persistent drainage of pus or blood from the anal opening
- Recurrent anal abscesses
- Skin irritation around the anus
- Pain that worsens with sitting or bowel movements
- Fever and general malaise (if infected)
- Swelling and redness around the anus
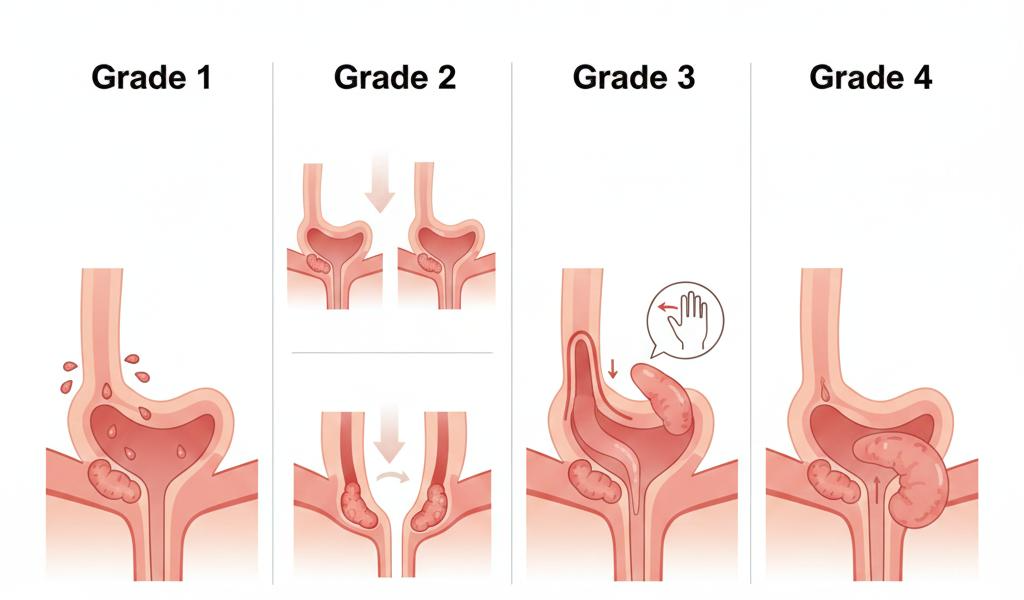
Piles Types & Stages:
Grade 1: Internal hemorrhoids that bleed but don’t prolapse
Grade 2: Prolapse during bowel movements but retracts spontaneously
Grade 3: Prolapse requiring manual pushing back
Grade 4: Permanently prolapsed, cannot be pushed back
Fissure Types:
- Acute fissures (recent onset, usually heal with medication)
- Chronic fissures (lasting 6+ weeks, may need surgery)
Fistula Types:
- Simple vs. Complex fistulas
- Based on the relation to the sphincter muscles
Risks of Piles, Fissure & Fistula – Why Early Treatment Matters
Piles, fissures, and fistula are common anorectal problems, but delaying treatment can increase the risk of complications and long-term discomfort. Piles (problem piles), if ignored, may lead to persistent bleeding (piles of blood), anemia, severe pain, and prolapse requiring surgery. Many patients keep searching for piles medicine, piles medicine name, or a hospital for piles near me, but self-medication without proper diagnosis can worsen the condition. Both male and female piles patients can experience worsening symptoms due to chronic constipation, poor diet, or prolonged sitting. Understanding the types of piles and choosing the right food for piles can help reduce reoccurrence. However, advanced cases require medical care from a specialist experienced in managing male or female piles.Piles, fissures, and fistula are common anorectal problems, but delaying treatment can increase the risk of complications and long-term discomfort. Piles (problem piles), if ignored, may lead to persistent bleeding (piles blood), anemia, severe pain, and prolapse requiring surgery. Many patients keep searching for piles medicine, piles medicine name, or a hospital for piles near me, but self-medication without proper diagnosis can worsen the condition. Both male and female piles patients can experience worsening symptoms due to chronic constipation, poor diet, or prolonged sitting. Understanding the types of piles and choosing the right food for piles can help reduce recurrence. However, advanced cases require medical care from a specialist experienced in managing male or female piles.
An anal fissure may start as a small tear, but untreated fissures can become chronic, causing severe pain, spasm, and fear of bowel movements. This often leads people to delay defecation, worsening constipation and increasing the risk of injury. Many patients search online for a fissure doctor near me or try home remedies, but chronic fissures may need proper medical or procedural treatment. Persistent pain and infection can significantly affect daily life and mental health if timely care is not taken.
An anal fistula carries the highest risk if neglected. What begins as a small infection can turn into a permanent unusual tract with continuous pus discharge, recurrent abscesses, fever, and spread of infection—sometimes leading patients to urgently search for a fever doctor near me. Unlike piles or fissures, a fistula does not heal with medicines alone, and delayed treatment increases the risk of complex surgery and recurrence. Traditional approaches like moolam treatment may offer temporary relief, but definitive medical or surgical management is often required.
Early consultation at a clinic near me or a specialized hospital ensures correct diagnosis, appropriate treatment, and lifestyle guidance. Whether it is choosing the right pills for medicine, understanding diet changes, or knowing when surgery is necessary, professional care prevents complications and improves quality of life. Awareness is especially important in regions where conditions like piles in Tamil (மூலம்) are common but often underreported due to hesitation or embarrassment.
Risk Factors:
Piles (Hemorrhoids)
Primary Risk Factors:
- Chronic Constipation or Straining
- Prolonged straining during bowel movements increases anal vein pressure
- Hard stools cause mechanical damage
- Low-Fiber Diet
- Insufficient dietary fiber leads to harder stools
- Common in processed food-heavy diets
- Prolonged Sitting
- Office workers, drivers, and sedentary lifestyles
- Increased pressure on the rectal veins
- Age-Related Tissue Weakening
- Supporting tissues weaken after age 50
- Natural collagen breakdown
Specific Population Risks:
- Pregnancy & Childbirth (Female Piles)
- Uterine pressure on pelvic veins
- Hormonal changes relax veins
- Straining during delivery
- Obesity
- Increased abdominal pressure
- Poor circulation in the pelvic region
- Often combined with a low-fiber diet
- Genetic Predisposition
- Family history of piles
- Inherited weak vein walls
Anal Fissure Risk Factors
Mechanical Causes:
- Traumatic Bowel Movements
- Passing large, hard stools
- Chronic diarrhea episodes
- Rough toilet paper use
- Anal Muscle Issues
- Overly tight sphincter muscles
- Muscle spasms post-injury
- Reduced blood flow to the anal region
Lifestyle & Medical Factors:
- Inflammatory Conditions
- Crohn’s disease
- Ulcerative colitis
- Chronic infections
- Childbirth Trauma
- Tearing during delivery
- Episiotomy complications
- Anal Intercourse
- Mechanical stretching
- Tissue trauma
Anal Fistula Risk Factors
Primary Causes:
- Previous Anal Abscess
- 50% of abscesses develop into fistulas
- Incomplete drainage
- Recurrent infections
- Inflammatory Bowel Disease (IBD)
- Crohn’s disease (30-50% develop fistulas)
- Ulcerative colitis complications
- Chronic intestinal inflammation
Secondary Risk Factors:
- Radiation Therapy
- Pelvic radiation damage
- Tissue necrosis
- Poor healing capacity
- Trauma or Surgery
- Previous anal surgery
- Accidental injury
- Foreign body insertion
- Infectious Diseases
- Tuberculosis
- HIV/AIDS complications
- Sexually transmitted infections
- Diverticulitis
- Colon inflammation spread
- Perforation complications
Who Are the Eligible Candidates for Treatment
Immediate Treatment Candidates:
- Those with persistent bleeding
- Severe pain affecting daily life
- Recurrent infections or abscesses
- Failed conservative treatment (like piles medicine)
- Complications like anemia from blood loss
- Quality of life was significantly impacted
Non-Surgical Candidates:
Those with mild symptoms may try:
- Piles medicine names like topical creams, suppositories
- Best food for piles – high fiber diet
- Warm sitz baths
- Stool softeners
Is Surgery Risky
Traditional Surgery Risks:
- Pain during recovery
- Bleeding risks
- Infection possibility
- Temporary incontinence risk
- Longer recovery time
Modern Laser Treatment Advantages:
- Minimal pain during and after the procedure
- Day care procedure (no hospitalization)
- Precision targeting with less tissue damage
- Reduced bleeding (laser seals blood vessels)
- Lower infection risk
- Faster recovery compared to traditional surgery
How Long Is Recovery
Non-Surgical Treatments:
- Resume normal activities the same/next day
- Minor discomfort for 1-2 days
Laser Procedures:
- Return to work in 1-2 days
- Mild discomfort for 2-3 days
- Avoid heavy lifting for 1 week
- Complete healing in 2 weeks
Traditional Surgery:
- Hospital stay: 1-3 days
- Significant discomfort: 1-2 weeks
- Return to work: 2-3 weeks
- Complete recovery: 4-6 weeks
Problems Come Back After Treatment
Piles, anal fissure, and anal fistula can come back after treatment if the underlying causes are not properly addressed. While modern treatments—especially laser procedures and minimally invasive surgeries—offer excellent success rates, long-term results depend greatly on lifestyle changes, bowel habits, diet, and follow-up care.
Piles (Hemorrhoids) may recur if chronic constipation, straining during bowel movements, prolonged sitting, or a low-fiber diet continues after treatment. Even after successful laser piles treatment or surgery, ignoring hydration, fiber intake, and regular bowel habits can lead to re-swelling of veins. However, recurrence rates are low when patients maintain a high-fiber diet, adequate water intake, and a healthy lifestyle.
Anal fissure recurrence is usually linked to the return of hard stools or constipation. Acute fissures heal well with medicines, but chronic fissures may reappear if dietary discipline is not maintained after treatment or surgery. Procedures like lateral internal sphincterotomy or laser fissure surgery significantly reduce recurrence, especially when combined with stool softeners and lifestyle modification.
Anal fistula, unlike piles or fissures, does not heal permanently with medicines alone. Recurrence can occur if the fistula tract is complex or not completely treated. Advanced techniques such as laser fistula treatment (FiLaC), VAAFT, or staged surgery reduce recurrence risk while preserving sphincter function. Proper diagnosis, experienced surgical care, and post-operative hygiene are crucial for long-term success.
In summary, while modern treatment options offer long-lasting relief, recurrence of piles, fissures, or fistula is possible without diet control, constipation prevention, weight management, and regular medical follow-up. Early consultation and preventive care play a key role in avoiding repeat problems.

Treating piles, fissures, and fistulas begins with an accurate diagnosis at a trusted clinic near me. For early-stage piles, your doctor may first recommend piles medicine (like topical creams or suppositories) alongside lifestyle changes, including a high-fiber diet for piles. If problems persist, numerous advanced, minimally invasive procedures exist.
For Piles: Treatments range from in-office procedures like rubber band ligation to modern laser treatment, which seals the hemorrhoid with minimal pain and faster recovery, often making it the best doctor-recommended option for suitable candidates.
For Fissures: The goal is to break the cycle of pain and spasm. This often starts with prescribed ointments and dietary management. For chronic cases, a minor procedure like Botox injection or a lateral internal sphincterotomy can provide lasting relief.
For Fistulas, Surgery is typically required to cure the abnormal tunnel. The approach—from fistulotomy to advanced LIFT or laser procedures—depends on the fistula’s complexity, always aiming to resolve the infection while preserving continence.

.png)



